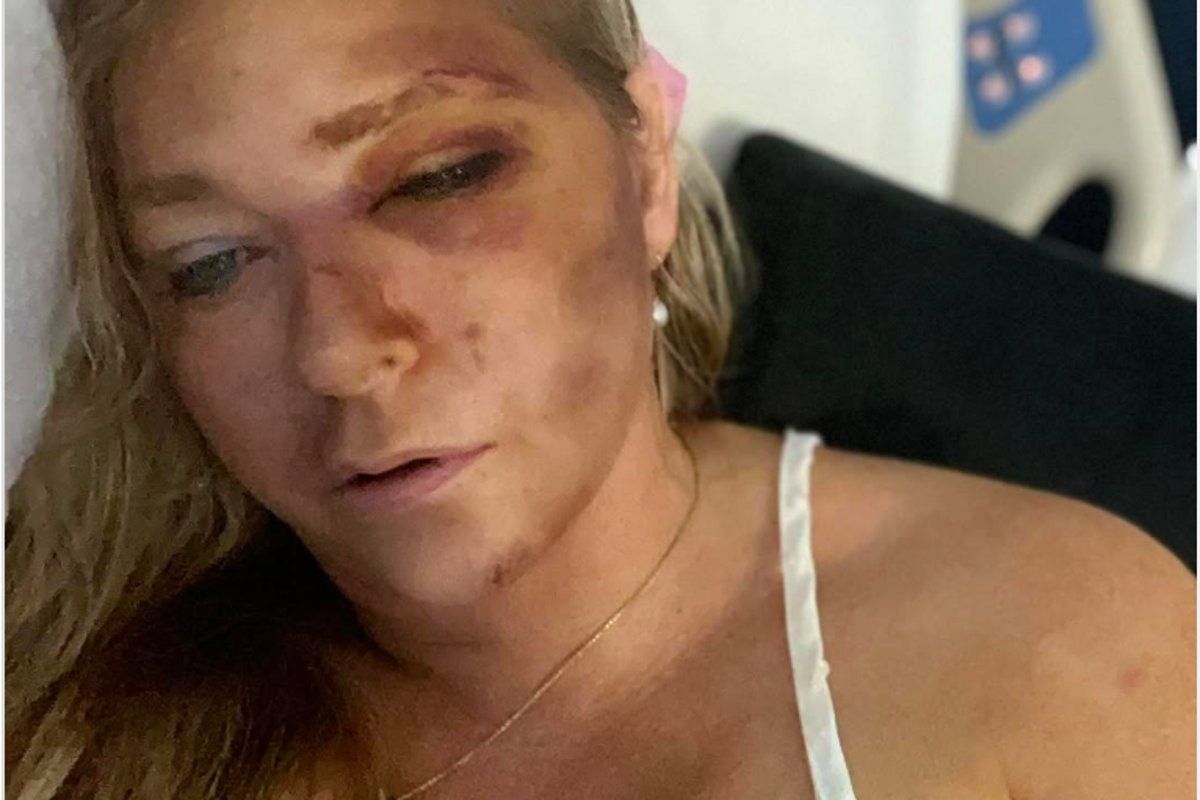
A woman who underwent surgery to remove a brain tumour while she was awake is looking forward to the future after the “life changing” operation.
Brooke MacFadyen’s tumour was discovered in May when she had an MRI after she went to her GP following a seizure.
In August, she underwent a highly specialised brain operation known as awake craniotomy, a procedure used to remove primary brain tumours.
The goal of the surgery is to remove as much tumour tissue as possible while minimising the risk of complications or longer-term effects on motor control and cognitive functions.
To do that Ms McFadyen was kept conscious during key parts of the surgery to help ensure the procedure was going to plan.
The 24-year-old needed to wait a few weeks after her operation to find out how serious the tumour was, but she has just been given the positive news that she and her family were hoping for.
She said: “I will be getting looked after with some future treatment to prevent the tumour coming back, but basically I can look forward now with real confidence.”
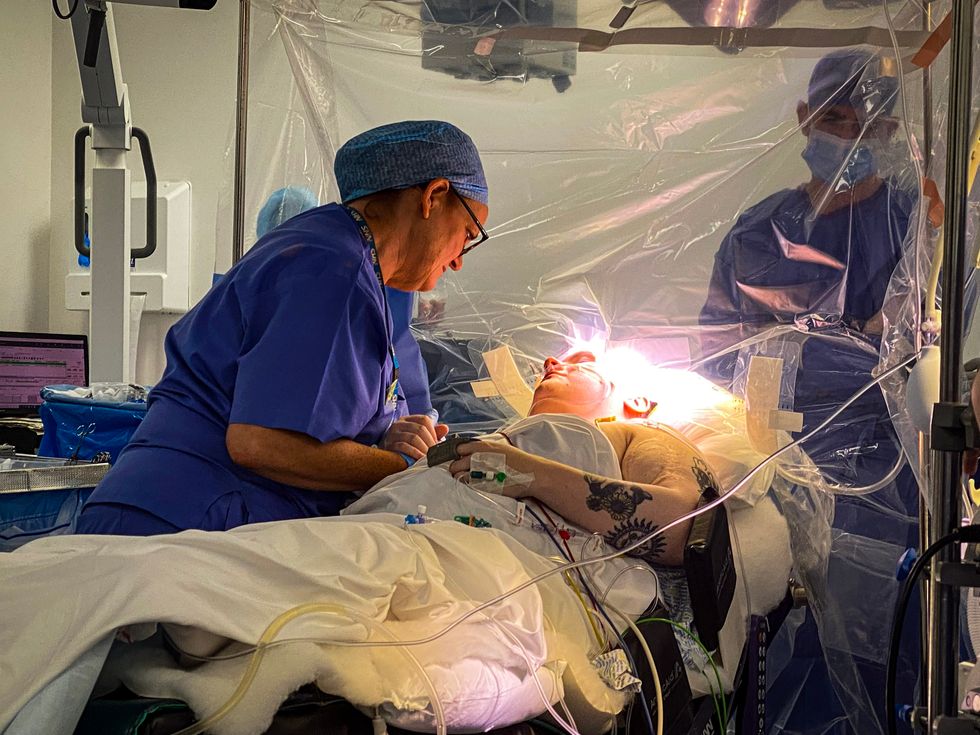
The medical team at the Institute for Neurological Sciences, part of the Queen Elizabeth University Hospital campus in Glasgow, used a new system called NeuroMapper – a digital platform that allows monitoring across a wider range of functions such as language, attention, working memory, visuospatial and executive functions, during the awake stage of the surgery.
During the operation, which took more than seven hours, staff operated the NeuroMapper and worked with the rest of the theatre team to gauge the patient’s reactions and ensure the procedure was going to plan.
Ms McFadyen, from Coatbridge in North Lanarkshire, said she was initially shocked to hear about awake craniotomy but is now looking forward to the future.
She said: “When I heard about the awake craniotomy, it took me a couple of weeks to get over the shock, but then I decided ‘I’m going to do this’.
“Strangely it’s been a really positive experience. I’ve been through life-changing surgery and now feel completely different.
“Before I doubted myself so much – I’d get into my own head with things, talk myself out of things. But not now – I now know I’m a really strong person, and super-independent.
“Making this decision – something I was so scared of – I’m going to use it as a positive from now on.”
NeuroMapper has real potential to be a revolution in intra-operative brain mapping, bringing real benefits for the surgical team, for the patient - and for longer-term outcomes
Dr Sharon Mulhern
The 24-year-old has already booked a holiday to Tenerife with a friend and is now determined to fulfil her dream of becoming a primary school teacher.
She thanked the team at NHS Greater Glasgow and Clyde who cared for her, saying: “From the doctors to the cleaners and the nurses on the ward, they are all special people to be able to do what they do – I’ll never forget what you’ve done for me.”
She also said a special thank-you to Dr Sharon Mulhern, consultant clinical psychologist and lead for regional neuropsychology services, who held her hand and kept her calm during the procedure, saying she was like a “second mum”.
Dr Mulhern said: “Awake craniotomy is a highly specialised procedure often working to extremely fine margins.
“It’s early days, but NeuroMapper has real potential to be a revolution in intra-operative brain mapping, bringing real benefits for the surgical team, for the patient – and for longer-term outcomes.”
Consultant neurosurgeon Likhith Alakandy, who carried out the operation, said: “I have found NeuroMapper to be a great addition to awake craniotomies. It provides an accurate and objective assessment of patients’ language and cognitive abilities, comparing it to their pre-operative function.
“By providing constant feedback, it allows the surgeon to push boundaries of tumour removal while preserving important neurological and cognitive function.
“Maximising tumour removal is known to improve survival in patients with intrinsic brain tumour, so it helps provide a better outcome in these patients.”